By: Samantha Foster (DPhil in Clinical Neurosciences, 2024)
Let’s start by talking about the water system in your house. Large pipes supply water into your house; these then branch into smaller pipes to reach your appliances, like your shower or toilet. Once you have used the water, it travels into small drainage pipes that feed into larger pipes, which take the used water away from your house.
The blood vessels in your brain work pretty much the same way. Blood is pumped from the heart to the brain, entering via large arteries. These large arteries divide into small arteries to reach the different areas of the brain. Once those regions have used that blood, it flows out via the small veins, which then feed into bigger veins that transport the blood back to your heart.
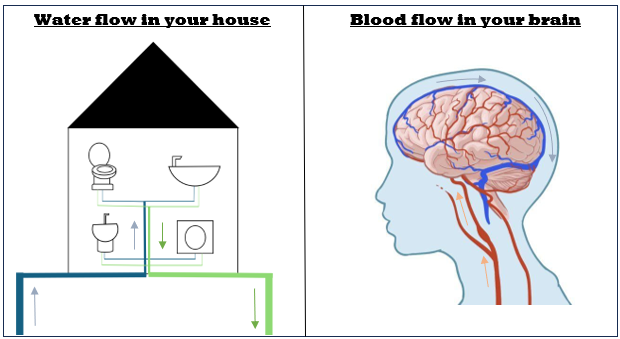
Blood Flow in your brain – Source: Osmosis. (2025). Cerebral circulation: Video, Causes, & Meaning | Osmosis. [online] Available at: https://www.osmosis.org/learn/Cerebral_circulation. Accessed on the 15th April 2026.
Sometimes the water pipes can get blocked, which prevents water from flowing. In the brain, blood vessels can become blocked, preventing blood flow, thereby causing an ischaemic stroke. Occasionally, water pipes can burst, which causes water to leak into your house. In the brain, blood vessels can rupture, leading to bleeding in the brain – these are referred to as haemorrhagic strokes.
In 2021, strokes were the leading cause of death and disability globally, and one in four adults will experience a stroke in their lifetime.1 80% of strokes are ischemic, and 20% are haemorrhagic. Within a month of haemorrhagic stroke, around 35% patients will die; in ischaemic stroke, this is approximately 11%.2,3
What causes the blockages in an ischemic stroke, and how do we treat them?
These blockages can be caused by fat built up over time, or a blood clot formed from a part of the body that has travelled up to the brain. To prevent ischaemic strokes in a person considered to have a high risk, doctors may prescribe blood-thinning medication to help improve the blood flow past these blocks or prevent clots from forming.
What about haemorrhages?
There are several causes, but one in particular behaves like rust in water pipes. Rust can build up over time, without you even noticing. Rust gradually weakens pipes and makes them more prone to rupturing. In the brain, a protein known as Amyloid-beta behaves similarly and builds up in the blood vessel walls. This disease is known as Cerebral Amyloid Angiopathy (CAA).
CAA accumulates with age and, over time, can cause significant damage to blood vessels. Unfortunately, there is currently no treatment to prevent CAA, and since it continuously builds up, an individual may experience more than one CAA-related haemorrhage.
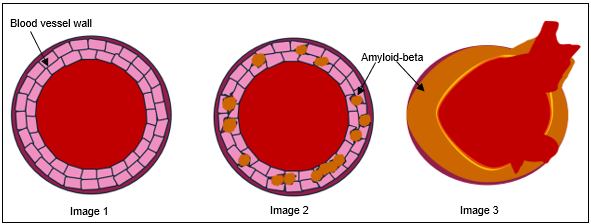
(Left to right) – Image 1: a healthy blood vessel. Image 2: Amyloid-beta protein is building up in the blood vessel wall. Image 3: a blood vessel with extensive CAA, which damages the blood vessel structure and causes blood to leak out.
Here, it gets a bit more problematic, as having one stroke does not prevent you from being at risk of another. So, this makes treatment very challenging for doctors. If we go back to the pipe analogy, having a blockage in a water pipe does not mean you are resistant to rust. Now to prevent a blockage, a plumber might alter the flow of water so that it can move past blockages more easily. However, if a rusty pipe is damaged and bursts, the water might travel further than before, causing much more damage to your house. This is a similar dilemma clinicians face when prescribing blood-thinning medication to patients with CAA, who are also at risk of ischaemic stroke; if the blood is thinner but a blood vessel ruptures, the blood will travel further and cause much more damage, which can be catastrophic.
So, what are the solutions?
To stop a catastrophic bleed, a doctor might stop blood-thinning medication altogether.
But what if the risk of having a blockage stroke is much higher than having a bleed?
Well, this is where my research comes in. I am investigating how common CAA is in patients who are at risk of or have had an ischaemic stroke. I aim to identify any factors that may help predict the likelihood of a future bleed. This will mean patients will not be withheld from potentially lifesaving treatment or given the wrong treatment.
How do we know who has the disease?
In rusty pipes, there may be signs before a big burst, for example, small spots of damp in the walls or a dripping tap. Small bleeds can occur on the surface of the brain, and these can be seen on brain imaging before a big bleed occurs.
I will be examining current diagnostic tests that recognise these signs to investigate whether there is a better way to identify patients with CAA and, therefore, improve our current approach to CAA diagnosis.
Although CAA can be devastating, not every person will have a haemorrhagic stroke. Different patients will progress at different rates and have varying levels of severity. I hope to provide some more certainty to patients with the disease and help them understand what their future may be.
But I must confess I am a neuroscientist, not a plumber (so do not take any of my blockage advice literally!).

| Source: Stroke Association (October 2023). World Stroke Day: Pass FAST on. Available at: https://www.stroke.org.uk/blog/world-stroke-day-pass-fast |
References
1. WHO. (2025) Stroke. [Online] Avaliable at: https://www.who.int/news-room/fact-sheets/detail/stroke. Accessed on 15th April 2026.
2. Tsao CW, et al. heart disease and stroke statistics—2023 update: a report from the American Heart Association. Circulation. 2023;147: e93–e621.
3. Dirren E, et al. Stroke Incidence, Case Fatality, and Mortality Using the WHO International Classification of Diseases 11: The Geneva Stroke Study. Neurology. 2025 Mar 11;104(5).
Sammy is a second year DPhil student and recipient of the Harriet and Joan Neal Scholarship for research into Cerebral Amyloid Angiopathy, kindly donated by Mike Neal. Her project focuses on Cerebral Amyloid Angiopathy in the context of stroke, with the aim of improving diagnosis and our understanding of the future of patients with this disease. Learn more about Sammy here.